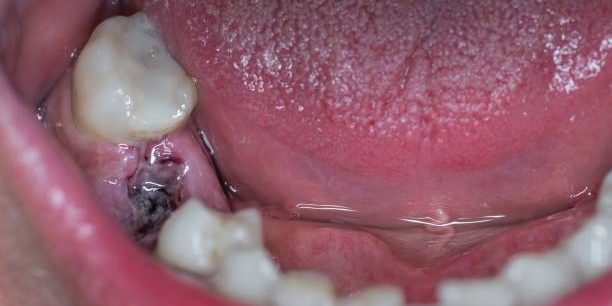
If you’ve searched “can dental implants cause cancer,” you’re not alone, it’s one of the most common concerns patients have before treatment.
The short answer is no, dental implants do not cause cancer based on current scientific evidence.
However, some rare cases of cancer have been reported near implants, which can sound alarming. This article explains what the research actually says, who may be at risk, and what you should realistically be aware of.
What Are Dental Implants, and What Are They Made Of?
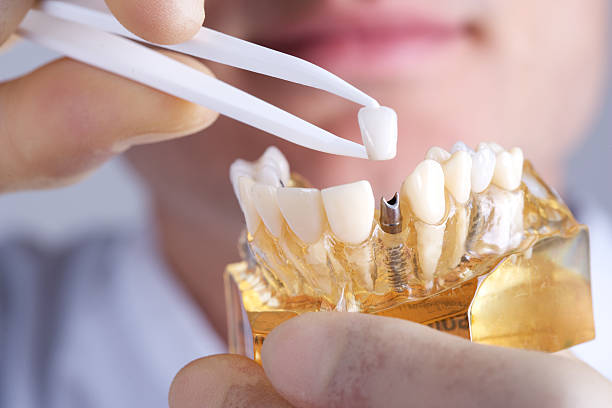
Dental implants, also called endosseous implants or osseointegrated implants, are titanium or zirconia fixtures surgically placed into the alveolar bone to replace missing teeth. They serve as an artificial tooth root, providing a stable foundation for a crown, bridge, or full-arch prosthesis such as an All-on-4 or All-on-6 restoration.
The vast majority of dental implants used in Australia are manufactured from commercially pure titanium (cpTi) or a titanium alloy (Ti-6Al-4V). Titanium is classified as a bioinert material, meaning it induces minimal adverse biological response in surrounding tissue. Upon contact with oxygen, titanium forms a protective titanium dioxide (TiO₂) oxide layer within milliseconds, a self-healing barrier that prevents the release of metallic ions into adjacent oral tissues.
All implant materials used in Australia must be approved by the Therapeutic Goods Administration (TGA) and comply with ISO 10993 biocompatibility standards before they can be used clinically.
In simple terms: Dental implants are artificial tooth roots made from highly biocompatible materials that safely fuse with your jawbone to support replacement teeth.
Read More: What Are Dental Implants? A Complete Guide to Tooth Replacement
What Does the Evidence Actually Say?
Current research shows no direct link between dental implants and cancer. Reported cases are extremely rare and usually involve patients with existing risk factors.
The Short Answer
Multiple systematic reviews and meta-analyses have concluded that no direct causal relationship exists between dental implants and the development of oral cancer. The clinical evidence, as it stands in 2026, does not support the idea that osseointegrated implants cause malignancy.
What the Research Shows
A comprehensive review published in 2026 identified around 105 reported cases of oral cancer near dental implants worldwide. To put this into perspective: millions of implants are placed every year, making these cases extremely rare. Importantly, most of these patients already had known risk factors such as pre-existing oral conditions or a history of cancer.
Critically, the authors noted that a significant proportion of these cases involved patients who already had oral potentially malignant disorders (OPMD), pre-existing conditions such as oral lichen planus, leukoplakia, or erythroplakia, or a prior history of OSCC. The review concluded that the available evidence does not support a causal role for implants and should be interpreted as “hypothesis-generating rather than inferential.”
An earlier systematic review published in the Journal of Oral Medicine and Oral Surgery similarly found that “it is not possible to establish a cause-effect relationship between dental implants and the development of OSCC.”
These findings are consistent across the literature. Dental implants are not carcinogenic devices.
So Why Do Some Cases Appear Near Implants?
This is where the science becomes more nuanced, and more important for patients to understand.
1. Field Cancerisation
The concept of field cancerisation refers to areas of the oral mucosa that have sustained genetic damage from carcinogens, most commonly tobacco and alcohol, making that tissue inherently more susceptible to malignant transformation. When an implant is placed in genetically altered mucosa, the proximity of a subsequent cancer to the implant fixture does not mean the implant caused it.
2. Chronic Peri-implant Inflammation
Peri-implantitis, the inflammatory condition affecting the soft tissue and bone surrounding a dental implant, shares clinical features with early OSCC. Chronic inflammation drives the release of pro-inflammatory cytokine mediators including interleukin-1 (IL-1), interleukin-6 (IL-6), prostaglandins, and tumour necrosis factor (TNF-α). In theory, sustained, unresolved inflammation in genetically vulnerable tissue could contribute to oncogenic cellular changes, but this remains a hypothesis, not a confirmed mechanism.
Importantly, peri-implantitis caused by inadequate oral hygiene, poorly fitted prostheses, or untreated periodontal disease is a known risk factor for implant failure, and potentially a cofactor in peri-implant soft tissue pathology in high-risk patients.
3. Diagnostic Masquerade
Several case reports in the literature describe OSCC initially misdiagnosed as peri-implantitis. This is a clinically important finding. If a peri-implant lesion does not respond to standard periodontal treatment, presents with unusual features such as rapid onset, tissue induration, altered sensation (paraesthesia or anaesthesia), or ulceration, a soft tissue biopsy should be performed promptly.
Early-stage OSCC is highly treatable. Delayed diagnosis because of a presumed inflammatory aetiology carries significant prognostic consequences.
Who Is at Real Risk?
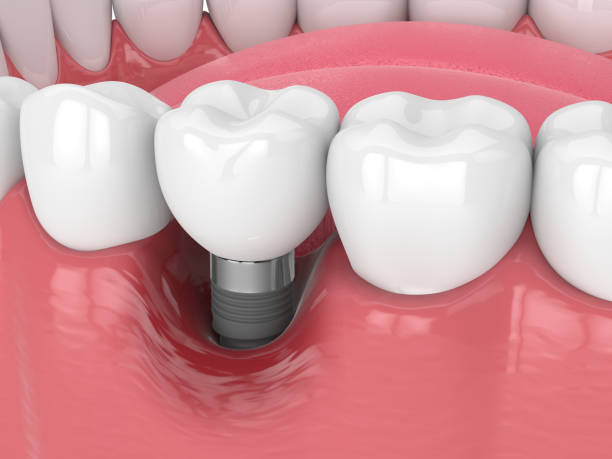
The evidence clearly identifies specific cohorts who carry elevated risk of peri-implant malignancy. These are not people for whom implants are contraindicated, but patients who require careful pre-operative assessment, informed consent, and close long-term monitoring:
- Tobacco smokers and heavy alcohol users: the two strongest independent risk factors for OSCC, regardless of implant status
- Patients with a prior history of OSCC or head and neck cancer: field cancerisation significantly increases recurrence risk in peri-implant mucosa
- Patients with diagnosed OPMDs: including oral lichen planus, leukoplakia, and erythroplakia; a 2025 systematic review in Dentistry Journal found implant survival rates remain high in OPMD patients (99.3% for oral lichen planus over 40 months), but surveillance remains essential
- Immunocompromised individuals: including those on immunosuppressant therapy or with conditions affecting immune surveillance
- Patients who have undergone head and neck radiotherapy: a 2025 meta-analysis in Clinical Oral Implants Research found implant survival rates were significantly lower in irradiated patients (85.6%) compared to non-irradiated patients (90.0%), and bone loss risk is elevated
Implant Safety in Australia: What Protects You
Australia has some of the most rigorous medical device regulations in the world. Patients considering dental implants in Sydney or elsewhere in Australia can take confidence from the following safeguards:
Therapeutic Goods Administration (TGA): All dental implant systems must be registered on the Australian Register of Therapeutic Goods (ARTG) before clinical use. The TGA requires biocompatibility testing, clinical evidence, and post-market surveillance.
Dental Board of Australia & AHPRA: Under the Health Practitioner Regulation National Law, all registered dental practitioners are required to provide care that is evidence-based, honest, and non-misleading. Advertising guidelines enforced by AHPRA (updated September 2025) require that all health claims, including those about implant safety, are accurate and substantiated.
ISO Standards: Implants used in Australian clinics must comply with ISO 10993 (biocompatibility of medical devices) and ISO 7405 (evaluation of biocompatibility of medical devices used in dentistry).
These overlapping layers of regulatory oversight mean that when you receive dental implant treatment from a registered practitioner in Australia, you are protected by multiple independent safety frameworks.
Warning Signs Every Implant Patient Should Know
Whether you have recently received implants or have had them for years, be aware of the following signs that warrant prompt clinical review, not because cancer is likely, but because early assessment is always the appropriate standard of care:
- A peri-implant lesion or swelling that does not resolve after 6–8 weeks of appropriate treatment
- Ulceration or irregular tissue growth around an implant site
- Unexplained numbness, tingling, or altered sensation (paraesthesia) in the jaw, lip, or tongue
- Rapid bone loss or implant mobility without clear cause
- Persistent pain unrelated to normal healing timelines
If you notice any of these symptoms, contact your dental practitioner immediately. They may recommend a soft tissue biopsy and/or referral to an oral and maxillofacial surgeon for specialist review.
You Might Like: What to Expect During the Dental Implants Procedure
The Bottom Line
Dental implants do not cause cancer based on current scientific evidence.
The extremely small number of reported cases are almost always linked to existing risk factors, not the implant itself. For most patients, dental implants are a safe, reliable, and well-regulated solution for replacing missing teeth. The key is proper assessment, good oral hygiene, and regular check-ups to ensure long-term success.
Disclaimer: This content is intended for general informational purposes only and does not constitute individual dental or medical advice. Individual patient outcomes vary. Please consult a registered dental practitioner for an assessment specific to your clinical situation.